What are wearable devices in healthcare?
Wearable devices in healthcare are tools worn on the body, such as smartwatches and fitness trackers, that continuously monitor health data like heart rate, sleep patterns, and activity levels. They are used for general wellness as well as managing chronic conditions, with medical-grade devices providing more specific and accurate information like ECG readings, glucose monitoring, and blood pressure. This technology enables proactive health management, early disease detection, personalized interventions, and remote patient monitoring, improving patient engagement and allowing for a more complete picture of an individual’s health over time.
Key uses and functions:
- Continuous monitoring: Wearables provide real-time data on vital signs, such as heart rate, blood oxygen, and body temperature, which is more comprehensive than traditional, one-off readings during doctor visits.
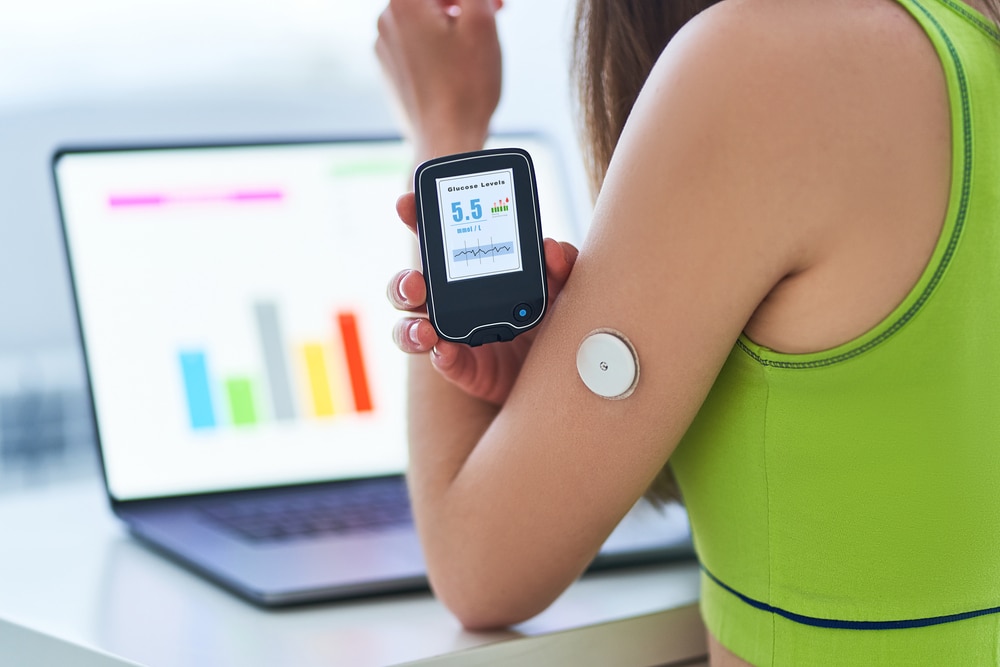
- Disease management: They are crucial for managing chronic conditions like diabetes and hypertension by providing continuous blood glucose and blood pressure data.
- Early detection and screening: Devices can screen for conditions like atrial fibrillation and sleep apnea by analyzing heart rhythms and sleep quality.
- Proactive health: With AI and machine learning, wearables can predict potential health issues, such as infections, before symptoms become severe.
- Remote patient monitoring: They allow healthcare providers to monitor patients remotely after surgery or for chronic diseases, reducing the need for in-person visits, especially for those in rural areas or with mobility issues.
- Personalized care: The data collected helps create more personalized health plans and allows for more accurate diagnoses and treatments.
Examples of wearable devices:
- Smartwatches: Devices like the Apple Watch can perform ECGs, monitor blood oxygen, and detect falls.
- Fitness trackers: Popular devices from brands like Fitbit track activity, sleep, and heart rate.
- Continuous Glucose Monitors (CGMs): Devices such as the Dexcom G6 and Freestyle Libre provide real-time blood sugar monitoring for people with diabetes.
- Smart rings: The Oura Ring offers discreet monitoring of heart rate, temperature, and sleep cycles.
- Medical-grade patches: Wearable patches, like the BioBeat patch, are used in hospital settings for remote patient surveillance and can track heart rate, blood pressure, and respiratory rate.
- Other devices: Other examples include smart rings that track sleep and recovery, and smartwatches with oximeters to detect sleep apnea.

Image: Shutterstock
UPDATED BY
Rose Velazquez | Sep 16, 2025
Wearable technology in healthcare aims to shake up the industry and empower patients with granular data that leads to actionable insights. With wearables, patients have the ability to collect their own health data and report it in a digital format, eliminating the need for in-person appointments. Insurers and providers have also bought into wearable technology, relying on data collected from health monitoring devices to inform more personalized and accurate health plans. Even companies have adopted wearables to encourage healthy habits among office workers and employees working from home.
What Is Wearable Technology in Healthcare?
Wearable technology in healthcare refers to devices that patients attach to their bodies to collect health and fitness data, which they may provide to doctors, health providers, insurers and other relevant parties. Examples include fitness trackers, blood pressure monitors and biosensors.
Because of these benefits, wearable medical devices — like fitness trackers, smart watches, electrocardiogram (ECG) monitors, blood pressure monitors and biosensors — have witnessed booming demand. The smart wearable health devices market was valued at $13.8 billion in 2020, and it’s expected to balloon to $37.4 billion by 2028.
An Overview of the Wearable Market in Healthcare
MarketsandMarkets suggests that the global market for wearable healthcare devices will approach $70 billion by 2028, with annual growth in the market exceeding 11 percent per year. Devices fall into two broad categories.
One is medical-grade wearables such as blood pressure, glucose and heart monitors. These devices undergo clinical research and must receive U.S. Food and Drug Administration clearance to gather data that will be used to support clinical decision-making. Common use cases for medical-grade wearables include monitoring patients at home after surgery or assisting patients with self-management of diabetes, hypertension or other chronic conditions.
The other category is consumer-grade wearables, which include watches, rings and articles of clothing. MarketsandMarkets notes that these devices account for the largest share of wearables. This stems from increased availability and accessibility of devices, interest in real-time self-monitoring of health and wellness, rising adoption of 5G, and the proliferation of smartphone apps for managing data.
That said, a 2022 literature review noted that the accuracy and reliability of device sensors poses a concern, in large part because consumer-grade devices aren’t subject to the same scrutiny as medical-grade wearables. Battery life may also pose a challenge, as sustained use is difficult if devices must be charged at least once a day. Older users may face further frustration due to small text, limited instructions and hard-to-use clasps or straps.
The Benefits of Wearables in Healthcare
The same literature review highlighted significant benefits for wearables in health and wellness management. Ongoing tracking helps patients set goals, while companion applications can provide context, offer tailored support and help patients better understand their conditions. Providers also get a more holistic view of patient health beyond what they report during short appointments.
This is all possible thanks to the use of open application programming interfaces (APIs). Devices such as Apple Watch and apps such as Apple Health “have the infrastructure behind them to get the data where it needs to be,” Taylor says. “It can be visualized for you as a patient to let you know it’s time to work out today, or it can be visualized within the electronic health record and used to make clinical decisions.”
There are two specific instances where MultiCare has had success with wearables. One is care management under risk-based contracting. This works well, Taylor says, because the economic model supports both the purchase of devices for patients and the staffing of care managers and remote monitors.
“We see a difference in outcomes with wrap-around care management,” she says. “Helping patients use the devices helps create good habits.”
Another instance is remote patient monitoring for patients struggling to manage chronic conditions. This has contributed to increased patient involvement in self-management and decreased readmissions associated with chronic conditions, says Chad Gabelein, MultiCare’s telehealth services director. (He notes that this effort is not part of the Centers for Medicare & Medicaid Services’ Acute Hospital Care at Home program.)
Here, too, care management plays a pivotal role in success. “We can’t just unleash the technology and think a primary care physician will monitor that,” Gabelein says. “It takes a lot of finesse, and you need the people power to support the actions associated with reviewing the data.”

Practitioners have to be able to react to trends, not just data. We need to drive automation in teasing out and trending values for patients.”
Chad Gabelein Telehealth Services Director, MultiCare
The Challenges of Wearables in Healthcare
That need for finesse gets to the heart of the challenges presented by the wider adoption of wearables. “The availability of data has almost exceeded our ability to manage it and use it to its most effective capacity,” Gabelein says.
Say a patient is discharged from the hospital after experiencing congestive heart failure. In theory, wearables could help monitor blood pressure and heart rate in real-time, ensuring that the patient is recovering well. In practice, Gabelein says, a health system would be asking a primary care provider already seeing more than 20 patients per day to review data streams of vital signs being generated 24/7.
“Practitioners have to be able to react to trends, not just data,” he adds. “We need to drive automation in teasing out and trending values for patients.”
Even if those types of analytics tools are available, organizations need the computing power to process them. That’s difficult to do with on-premises systems, Taylor says: “Being able to compute the data and use AI is pure electricity.” She adds that this may motivate a health system to migrate to a cloud-based electronic health record.
The sheer volume of wearables, especially in the consumer-grade market, also poses an obstacle. No organization can account for every open API needed to integrate wearables with clinical systems, and few have the staff to manage those integrations.
Security priorities must be shifted as well. Taylor recommends an emphasis on device identity management and verification at the point of care.
The Future of Wearable Technology in Healthcare
Amid these concerns, a 2022 paper provided four recommendations for supporting more effective use of wearables in healthcare:
- Context-based data quality standards: False positives are OK for fitness tracking but should be limited for remote monitoring of vital signs and all but eliminated for diagnostics.
- Interoperable data: Not only does this address concerns about data ingestion and storage, it also makes standards easier to apply — for example, by enabling comparisons of devices from different manufacturers.
- Access to data and analytics tools: Eliminating barriers to accessing information and insight from wearables increases the likelihood of long-term adoption.
- A more representative user base: As the populations most likely to benefit from wearables are often the least likely to use them, the industry should strive to promote the benefits of wearables for wellness, not just health monitoring.
Additional research has pointed to the potential for wearables to address issues of inequity in maternity care, where an estimated 80 percent of instances of morbidity and mortality are preventable, and to broaden participation in early-stage clinical trials, especially among populations traditionally excluded from clinical research.
Ultimately, Gabelein says, organizations are more likely to succeed with wearables when their strategy looks beyond the devices themselves.
“You have to associate wearables and their data with artificial intelligence. You have to evaluate the different inputs that are associated with the different devices,” he says. “The AI overlay helps you identify the most effective and necessary data, so you can be conscientious about the amount of meaningful data you send to clinicians.”